Case Study: Designing a Scrappy Intake & Referral Workflow at an Early-Stage Mental Health Startup

The Problem
A mental health startup receives referrals from counselors and families, but not all patients are covered by the company’s accepted insurance plans. These cases often require manual triage, leading to delays in care, inconsistent follow-up, and operational strain on a small team without any documentation of requests.
The goal was to design a lightweight, human-centered workflow that:
Responds to patients quickly
Reduces manual work for clinical and ops teams
Maintains trust with referral partners
Scales without heavy engineering investment
My Approach
I designed an automated intake + referral triage workflow using no-code tools like Make.com, prioritizing speed, clarity, and empathy.
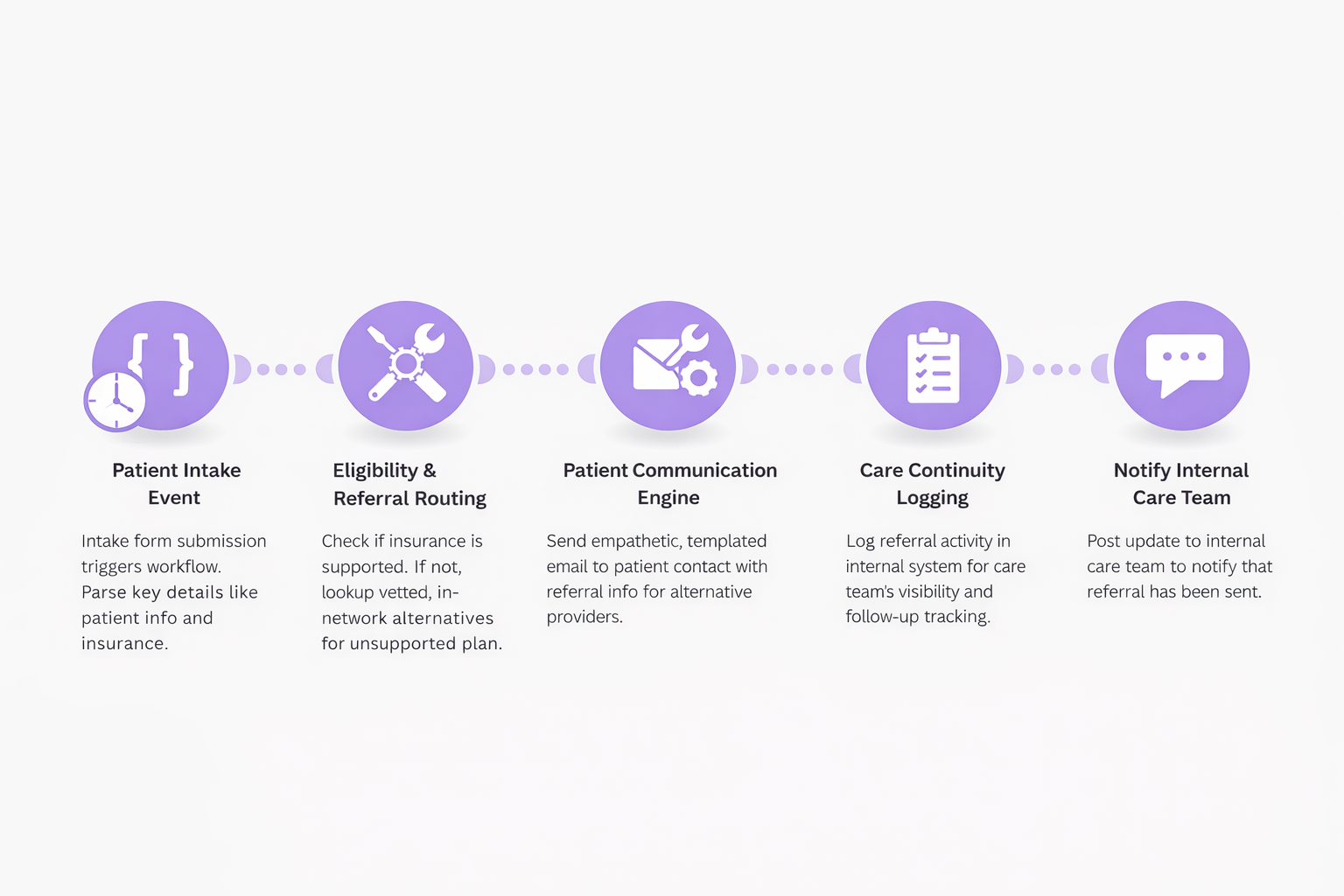
1. Intake Trigger
Intake data is submitted via a simple Google form (e.g. from a counselor or internal referral).
The workflow parses key fields like patient contact info, specialty, and insurance type.
2. Insurance Eligibility Check
The system checks whether the insurance plan is in network.
If the plan is not accepted, the workflow routes the case into an alternate referral path instead of dropping it into a backlog.
3. Provider Lookup (Out-of-Network)
A maintained spreadsheet/database is used to identify vetted, in-network providers who accept the patient’s insurance.
Providers are prioritized based on:
Specialty match
Availability
Prior relationships or team recommendations
4. Automated, Human-Toned Communication
A templated but empathetic email is automatically sent to the patient or guardian:
Acknowledging the referral
Explaining coverage limitations clearly
Providing a curated list of next-best providers
The language is designed to reduce confusion and reinforce that the company is still advocating for the patient’s care.
5. Internal Visibility & Logging
The workflow logs the referral outcome in the CRM/EHR for continuity.
A Slack notification alerts the clinical or ops team that follow-up was sent, maintaining visibility without manual pings.
Why This Works for a Scrappy Team
Fast to ship: Built with no-code tools and spreadsheets means there are no engineering dependencies.
Scalable: Handles higher referral volume without increasing ops headcount.
Patient-first: No silent drop-offs, every referral gets a response and every patient feels cared for.
Data-generating: Creates a clean record of out-of-network demand to inform future insurance contracting decisions.
What I’d Do Next (If This Were Live)
Analyze volume of out-of-network cases to build a business case for insurance partnerships
Add conditional logic for self-pay or bridge care options
Develop lightweight internal tool as volume grows